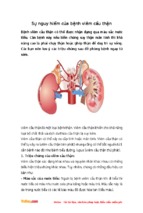
Mô tả:
Suy tim mạn:
GÓC NHÌN TỪ ACC 2017
PGS TS Châu Ngọc Hoa
Bộ môn Nội ĐHYD Tp HCM
ACC Focused update on HF, 2017
Two New Pharmacological Therapies
Approved by FDA for Heart Failure
• Ivabradine (April 15, 2015)
• Sacubitril/Valsartan (July 7, 2015)
WHO, WHEN AND WHY ADD
ON IVABRADINE
Ivabradine approval timeline
• 2005 approved in EU for angina
• 2012 approved in EU for heart failure
• 2015 approved in US for heart failure
to reduce the risk for hospitalization for worsening heart failure in patients with
stable, symptomatic chronic heart failure with LVEF ≤35%, who are in sinus rhythm
with a resting heart rate of ≥70 beats per minute (bpm) and are taking maximally
tolerated doses of beta-blockers or have a contraindication to beta-blockers.
Ivabradine
Blocks If channel
Slows heart rate
Few if any other CV effects
SHIFT Trial
> 6500 HF patients (NYHA II-IV)
LVEF < 35%
Resting HR > 70 BPM
Primary endpoint: composite of CV death/HF hospitalization
On maximally tolerated beta-blocker
SHIFT: primary outcome
CV death or hospitalization
40
for HF (%)
HR= 0.82
p<0.0001
Placebo
30
lvabradine
20
10
Months
6
12
18
24
Swedberg K., et al. Lancet.2010;376:875-885
SHIFT: HF hospitalization
Hospitalization for HF (%)
Placebo
30
HR= 0.74
20
10
6
12
18
24
30
Months
Swedberg K, et al. Lancet. 2010;376:875-885.
Ivabradine in HF
Up-titrate beta blocker dose as much as possible
Add on therapy to beta blocker; not replacement
Does not lower blood pressure
Contraindicated in atrial fibrillation
Benefit greater in patients with higher baseline heart rate
Target doses as defined in the ESC guidelines
Startingdose(mg)
Targetdose(mg)
Enalapril
2.5b.i.d
10-20b.i.d
Lisinopril
2.5-5.0o.d
20-35o.d
Ramipril
2.5o.d
5b.i.d
Bisoprolol
1.25o.d
10o.d
Carvedilol
3.125b.i.d
25-50b.i.d
Metoprololsuccinate
12.5/25o.d
200o.d
Eplerenone
25o.d
50o.d
Spironolactone
25o.d
25-50o.d
5b.i.d
7.5b.i.d
ACEI
Beta-blocker
MRA
IfInhibitor
Ivabradine
Can we reach and maintain „target” dose
in „real-life” elderly HF patients with comorbidities ?
CIBIS-ELD – 883 elderly HF patients;
The primary endpoint: tolerability, defined as reaching and maintaining guidelinerecommended target doses after 12 weeks treatment.
Dungen HD, et al. Eur J Heart Fail. 2011:13:670–680.
Up-titration period as defined in the landmark trials
Trials
Targetdose (mg)
Time to reach target/max tolerated dose
ACEI
Enalapril
SOLVD
10b.i.d
Notspecified
Lisinopril
ATLAS
35o.d
4weeks
CIBISII
10o.d
11weeks
25b.i.d
6weeks
Metoprololsuccinate MERITHF
200o.d
6weeks
Nebivolol
10o.d
6weeks
50o.d
4weeks
7.5b.i.d
2weeks
Beta-blocker
Bisoprolol
Carvedilol
COPERNICUS
SENIORS
MRA
Eplerenone
EMPHASIS-HF
IfInhibitor
Ivabradine
SHIFT
1- The SOLVD Investigators. N Engl J Med.1991;325:293-302. 2- Packer M, et al. Circulation. 1999;100:2312-2318. 3- CIBIS-II study group.
Lancet.1999;353:9-13. 4- Packer M, et al. Circ. 2002;106:2194-2199. 5- Merit-HF study group. Lancet.1999;353:2001- 2007. 6- Zannad F, et al.
N Engl J Med. 2011:364:11-21. 7- Swedberg K, et al. . Lancet 2010;376: 875-885.
Uptitration target in stable HF patients
ACEIs
4 weeks
Beta-blockers
6 weeks
Dose
MRAs
4 weeks
Ivabradine
2 weeks
.
Reasons for non-reaching target dose
CIBIS-ELD: RCT aimed to reach guideline-recommended target doses
883 HF patients, NYHA II-IV, >65 y, no contraindication or intolerance to BB
Dungen HD, et al. Eur J Heart Fail. 2011:13:670–680.
Yes but …
My Patient …
- is too old
- has low blood pressure
- has COPD
- has renal impairment
- is too sick
Treatment Effect of Ivabradine
According to Blood Pressure
Komajda M, et al. Eur Heart J. 2013;34 (Abst. Suppl), 610.
Patients (%)
Effect of ivabradine on composite of
CV death or HF hospitalization
50
45
40
COPD (placebo)
COPD (ivabradine)
35
30
Non-COPD (placebo)
Non-COPD (ivabradine)
25
20
15
10
5
N at risk
0
0
6
12
18
24
Time (months)
COPD (pl)
372
298
250
209
110
COPD (iva)
358
312
266
216
124
NCOPD (pl)
2892
2570
2239
1852
979
NCOPD (iva)
2883
2616
2334
1957
1067
Tavazzi L, et al. Eur Heart J. 2013;34 (Abst. Suppl), 652.
Patients (%)
Effect of ivabradine on composite of CV
death or HF hospitalization
50
Placebo, renal dysfunction
40
Ivabradine,renal dysfunction
Placebo, no renal dysfunction
30
Ivabradine, no renal dysfunction
20
10
N at risk
0
0
6
12
18
24
30
Time (months)
RD (pl)
799
706
612
488
261
95
RD (iva)
780
720
612
489
273
104
NRD (pl)
2293
2119
1847
1551
820
343
NRD (iva)
2288
2166
1963
1662
906
339
Voors A, et al. Eur Heart J. 2013;34 (Abst. Suppl).
Effect of early treatment of Ivabradine with BBs vs BB alone in
patients hospitalized for WHF: randomized ETHIC study
n=71 patients hospitalized for WHF
Greater improvement in LVEF
P=0.039
55.
Ivabradine + BB
BB alone
44.8
LVEF, %
46.
38.1
P=0.039
37.
32.9
29.8
29.9
31.9
28.
19.
10.
Admission
Dicharge
4 months FU
Hidalgo FJ et al. Int J Cardiol. 2016;217:7-11
- Xem thêm -