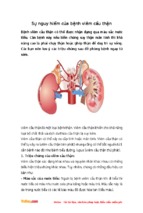
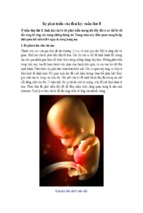
Mô tả:
Quality Management Systems (QMS)
in ART - How, Why & Who?
1
INTRODUCTION:
LEARNING OBJECTIVES
Identifying the
benefits
Objective 3.
Outlining
Quality
Control &
Quality(QC)
Assurance(QA)
procedures in
ART
Objective 2.
Objective 1.
Understanding
the concept of
Quality in ART
2
HOW?
3
Quality Management Standards are based on eight
quality management principles
4
EXAMPLE of QMS PROCESS –
Factual Approach to Decision Making
Initial
Information
Investigation
Treatment
Follow-up
5
QUALITY CONTROL & QUALITY ASSURANCE
The terms “quality assurance” and “quality control”
are often used interchangeably to refer to ways of
ensuring the quality of a service or product.
The terms, however, have different meanings.
6
QUALITY CONTROL
CONTROL:
An EVALUATION to INDICATE NEEDED CORRECTIVE RESPONSES;
the act of guiding a process in which variability is attributable to a constant
system of chance causes.
QUALITY CONTROL:
The OBSERVATION TECHNIQUES and ACTIVITIES used to fulfil
requirements for quality.
7
QUALITY ASSURANCE
ASSURANCE:
The ACT of GIVING CONFIDENCE, the state of being certain or the act of
making certain.
QUALITY ASSURANCE:
The PLANNED and SYSTEMATIC ACTIVITIES implemented in a quality
system so that quality requirements for a product or service will be fulfilled.
8
QUALITY ASSURANCE &
QUALITY CONTROL
9
QUALITY in A.R.T.
Determine which factors may affect the ART services,
both the processes involved in delivering the services
and the outcomes.
Clear idea of
the variables
10
KEY PERFORMANCE INDICTATORS
Set the Key Performance Indicators
BATCH NUMBERS
TOLERANCE LEVELS
Recording
Acceptable
Consumables
Culture medium
EPU needles & ET catheters
Drugs used in Ovarian Stim.
Any item used in IVF
Temperature Range
pH
CO2 levels
LN2 levels
Non embryotoxic
11
KEY PERFORMANCE INDICTATORS
EMBRYOTOXICITY
• Safety of all
products
that come in
contact with
gametes or
embryos
TEMPERATURE
• Control at
every phase
of culturing
pH
• Gas
environment
SAFETY
• Culturing
conditions
maintained
• Culture
medium
storage
12
QUALITY CONTROL MEASURES:
Temperature
pH
Gas supplies
LN2 levels
Emergency backup
Alarm systems
• Incubators, microscopes, refrigerators
• Fluids containing gametes / embryos
• Culturing fluids
• Incubator readings
• Gas mix & quality of cylinder
• LN2 loss from tanks – integrity of tanks
• Oxygen displacement alarms
• Emergency power – generators / UPS
• Battery power to alarms
• Test response systems regularly
• Trigger alarms
Embryotoxicity
• Culture medium - EQA
• Disposables – Lot. Nos. (dishes, tubes, gloves)
Contamination
• Culture plates for infection
• Culture medium
13
Air Purity - VOC
• VOC levels
• Air filter function
QUALITY CONTROL - EXAMPLE
Oocyte Temperature Process Map
Oocyte in
follicle
Oocyte
aspirated
to test tube
Test tube in
heating
block prior
to ID
Oocyte
inseminated
on m/scope
stage
Oocyte
cultured in
incubator
to D1
Cleavage
check on
m/scope
stage
D3 – embryo
moved to
blastocyst
medium
Oocyte in
dish on
warm stage
Fertilization
check on m/
scope stage
Embryo
moved to
ET dish
Oocyte
transfer to
culture dish
Oocyte dish
transferred
to
incubator
Embryo
moved to
CM in new
dish
Oocyte
culture in
incubator
D2
Embryo
loaded into
catheter
Embryo
transferred
into uterus
Legend:
AUDIT
Blastocyst
vitrified
14
Embryo in LN2
Tank
RISK
PROCESS
QUALITY ASSURANCE MEASURES:
Oocyte numbers
Oocyte Maturation rates
Fertilisation rates
ICSI Lysis rate
Pregnancy rates
Implantation rates
Miscarriage rates
Embryo Development Rates
• Competency of embryologist
• Competency of clinician
• Timing of egg retrieval
• Culturing conditions
• Sperm preparation – ICSI option
• Competency of ICSI skills
• Embryo transfer technique
• Culturing conditions
• Culturing conditions
• Temperature & pH control at time of egg collection
• Temperature & pH control
• VOC / contaminant levels
• Culturing conditions
• Culture medium
15
Live birth rates
• Culturing conditions
• Treatment selection
BENEFITS
of QMS
–
BENEFITS
of QMS
–
Identification
& Review
of Critical
IDENTIFICATION
& REVIEW
OF CRITICAL
PARAMETERS
(Q.C.
& Q.A.)
Parameters
(Q.C.
& Q. A.)
Develop process to identify nonconformities
Determine the causes of these
problems or variations
Evaluate actions to prevent a
recurrence
Determine and implement the
action necessary to address the
issue
Record action taken and results
Review these actions to ensure
the matter is satisfactorily
addressed
Decreases in
Fertilisation rates
Pregnancy rates (+βhCG; clinical)
Live birth rates
No. of eggs retrieved
Increased miscarriage rates
Blastocyst development
Utilisation rates
Frozen embryo survival
Revenue per cycle
Increase in
Customer complaints
OHSS rates
Infections
Multiple pregnancy 16rates
Business costs
QUALITY ASSURANCE - RESOURCES
Determine the resources necessary
to achieve the ART clinic objectives
/ KPIs.
17
QUALITY ASSURANCE - RESOURCES
1. Staff required to deliver service
18
RESOURCES – STAFFING REQUIREMENTS
Team
Player
Based on ART Clinic values
Embryologists
required per IVF
cycle –
1 embryologist
per 150 - 200
cycles
Attention to
detail
Technical
capabilities
Empathy towards patients
& staff; customer focussed
Good communication skills
IT skills
Responsible, dedicated & hard working
19
Organised
QUALITY ASSURANCE - RESOURCES
2. Physical resources required to
deliver service
Buildings; equipment; environs (e.g. ample space & equipment to
undertake cases; air-conditioning; emergency back-up)
Validate equipment to ensure suitability
Introduce calibration and maintenance processes to ensure
ongoing reliability & safety of equipment
20
- Xem thêm -