Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
5672 〈1102〉 Immunological Test Methods / General Information
Add the following:
■
〈1102〉 IMMUNOLOGICAL TEST
METHODS—GENERAL
CONSIDERATIONS
INTRODUCTION
This general information chapter provides a high-level
description of principles for immunological test methods
(ITMs) that can be used in specified monograph tests, along
with information and approaches to analytical development
and validation for ITMs. The scope of this chapter is to provide general information that is applicable to all ITMs. The
chapter provides a foundation for specific chapters about
different types of ITMs, e.g., Immunological Test Methods—
Enzyme-Linked Immunosorbent Assay (ELISA) 〈1103〉, Immunological Test Methods—Immunoblot Analysis 〈1104〉 (proposed), and Immunological Test Methods—Surface Plasmon
Resonance 〈1105〉. This suite of general information chapters
is related to the bioassay general information chapters. Use
of ITMs for process monitoring, diagnosis, and evaluation of
clinical response, assessment of pharmacokinetics/pharmacodynamics/absorption, distribution, metabolism, and excretion (PK/PD/ADME), and other product characterization
(nonrelease testing) is outside the scope of this chapter.
The basis of all ITMs used to measure a quality attribute
of a biologic drug substance or drug product is the highly
specific noncovalent binding interaction between an antibody and antigen. The antigen typically is an analyte of
interest (e.g., protein, carbohydrate, virus, or cell), and the
binder is usually an antibody (e.g., monoclonal antibody or
polyclonal antiserum). ITMs are applicable to molecules that
are either directly antigenic (immunogens) or can be rendered indirectly antigenic (haptens). The measurand in ITM
is directly related to a quality attribute of the product under
test.
ITMs are valuable because they exhibit high sensitivity
and specificity for an analyte in complex matrices. They typically are used for qualitative and quantitative assessment of
both an antibody and antigen, but their application also
extends to the measurement of hapten, complement, antigen–antibody complexes, and other protein–protein interactions. These properties of ITMs allow their use for assessing identity, potency (strength), purity, impurities, stability,
and other quality attributes of biological drug substances
and drug products.
ITMs are useful for many applications because they can
measure molecules over a wide range of sizes and binding
types. In general, antibodies are stable during various chemical modifications that do not have a significant adverse influence on interactions with an antigen. Antibody molecules
tend to withstand moderate acidic and alkaline pH changes
better than other proteins do. Because of this characteristic,
a variety of ITMs with high degrees of sensitivity and specificity are possible. The ability to accelerate contact between
an antigen and antibody enables ITM formats that provide
rapid or real-time results.
Generally, ITMs have higher precision and shorter turnaround time than do traditional biologically-based (i.e., cellbased and animal) assays. Although in some cases these advantages can support the replacement of a biological assay
with an immunoassay, such changes should be approached
systematically and with caution. Often it is challenging to
prove the equivalence, or comparability, of results from bioassays and immunoassays because the interaction between
antigen and antibody may not reflect the functional attributes observed in bioassays.
Second Supplement to USP 35–NF 30
One major limitation of ITMs compared to physicochemical methods (such as liquid or gas chromatography) is that
the latter generally are more precise and can simultaneously
identify a set of impurities or unexpected substance(s). Another major limitation is that generally ITMs operate at high
molar dilutions at which they are sensitive to disturbances
caused by environmental factors in the sample matrix (i.e.,
matrix effects). Matrix effects can depend on ITM format
and are not fully understood. Their specificity, a hallmark of
ITMs, is sometimes compromised by structural or sequence
similarities between the analyte and a closely related molecular impurity (cross-reactivity).
Most ITMs reflect physical interaction (binding) between
an antigen and antibody and not the analyte’s functional
properties. Therefore, analysts must pay attention in the selection and execution of ITM format. Cell-based ITMs that
can provide functional information about the analyte are beyond the scope of this chapter.
GENERAL CHARACTERISTICS OF ITMs
ITMs are based on the principle of specific, noncovalent,
and reversible interactions between an antigen and antibody. In general, the primary antigen–antibody reaction is
brought about by complementarity, which creates
macromolecular specificity. This noncovalent interaction determines the degree of intrinsic affinity. Intrinsic affinity contributes to functional and/or relative affinity that depends on
factors like reaction phase and valency, which in turn determines the degree of reversibility of an interaction. A better
understanding of factors that affect antigen–antibody interactions provides the rationale for the development of a suitable ITM format (e.g., solid or liquid phase, competitive or
noncompetitive binding, etc.).
A defining characteristic of ITMs is that they employ an
antigen (or hapten) and antibody. In addition, ITMs may
contain companion molecules such as complement components. The components of ITMs are defined as follows:
• Antigens—Comprise a wide range of molecules that
are capable of binding to the antibody in a specific interaction. Generally, part(s) of an antigen (the immunogenic epitope[s]) is/are capable of eliciting antibody
response.
• Haptens—Small molecules that, by themselves, are not
capable of eliciting an antibody response but are capable of eliciting an immune response when attached to a
large carrier such as a protein. Antibodies produced to
a hapten–carrier adduct also may bind to the smallmolecule hapten in a specific interaction.
• Complements—Companion molecules that, under certain conditions, aid in the functionality of antigen–antibody complexes but are not required for antigen–antibody or hapten–antibody interaction.
• Antibodies—Proteins with regions that impart a high
degree of specific binding to antigens (and haptens).
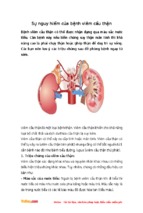
The structural elements of an immunoglobulin G (IgG)
antibody are shown in Figure 1.
In addition to these components, ITMs require some
means to detect or monitor the binding reaction between
the antigen and antibody.
TYPES OF ITMs
Measurement of antigen–antibody binding can be performed in a variety of assay types and formats: solid or liquid phase, manual or automated, labeled or nonlabeled,
competitive or noncompetitive, qualitative or quantitative,
homogeneous or heterogeneous, or combinations of some
of these. The distinguishing characteristic of all these assays
is the binding of an antibody or antigen to the analyte
(which can be an antigen or antibody as well), followed by
detection of the antigen–antibody complex. Although many
different formats can be used for the binding reaction,
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
Second Supplement to USP 35–NF 30
General Information / 〈1102〉 Immunological Test Methods 5673
Figure 1. The structure of IgG. The IgG molecule is characterized by a distinctive domain structure of heavy (H) and light (L)
chains, both of which are divided into variable and constant regions (V and C, respectively). Light chains consist of VL and CL
domains, and heavy chains consist of a variable domain (VH) and three constant domains (CH1, CH2, and CH3). All domains
are stabilized by disulfide bonds, and CH2 domains contain carbohydrates. The flexible hinge region between the CH1 and
CH2 domains allows the independent behavior of two antigen-binding sites formed by variable domains.
along with different methods for detection, quantification of
the analyte in the test article is always performed by comparison of the measurement to a reference standard. Thus a
number of ITM technologies support investigations of product quality. Commonly used assay designs include enzymelinked immunosorbent assay (ELISA), Western blotting, flow
cytometry, competitive enzyme-linked immunosorbent assay, surface plasmon resonance (SPR), rate nephelometry,
radioimmunoassay (RIA), radial immunodiffusion, precipitation, and agglutination. These methods are described
below.
Enzyme-Linked Immunosorbent Assay
An ELISA is a quantitative, solid-phase immunological
method for the measurement of an analyte following binding to an immunosorbent and its subsequent detection using enzymatic hydrolysis of a reporter substrate either directly (analyte has enzymatic properties) or indirectly (e.g.,
horseradish peroxidase– or alkaline phosphatase–linked antibody subsequently bound to the immunosorbed analyte).
The analyte usually is quantitated by interpolation against a
standard curve of a reference material. General information
chapter Immunological Test Methods—Enzyme-Linked Immunosorbent Assay (ELISA) 〈1103〉 discusses ELISA in greater detail, including ELISA development for quantitative analysis.
Western Blotting
A Western blot is a semiquantitative or qualitative method
for measurement of a protein analyte that has been resolved
by polyacrylamide gel electrophoresis and subsequently
transferred to a solid membrane (e.g., nitrocellulose, nylon,
or polyvinylidene difluoride). Detection can be achieved directly by reacting with a labeled primary antibody (antibody
specific to the analyte of interest) or indirectly by reacting
labeled secondary antibody (antibody against the primary
antibody) to the primary antibody bound to the membraneimmobilized antigen. The label can be a radioisotope or an
enzyme that uses the substrate to produce color, fluorescence, or luminescence. This method is semiquantitative, especially when proteins are present in low concentration and
in very complex mixtures. It is commonly used in early process development (e.g., antibody screening, protein expression, protein purification, etc.). Western blotting is a powerful method for analyzing and identifying proteins in
complex mixtures, particularly after separation using 2-dimensional gel electrophoresis, which separates proteins
based on size and charge (pI).
Flow Cytometry
Flow cytometry is a laser-based semiquantitative technology that permits measurement of fluorophore-conjugated
probes as they interact with their respective ligands on cells
or particles. More details for flow cytometry can be found in
Flow Cytometry 〈1027〉.
Surface Plasmon Resonance
SPR is a quantitative method for measurement of an
analyte in a sample where the antibody–antigen complex
formation can be measured in real time at the interface of a
liquid and solid (e.g., gold surfaces or particles). The measurement taken is the real-time change in refraction of a polarized light and occurs during the formation of the antibody–antigen complex, resulting in changes to the
plasmon resonance minima (i.e., the sensorgram). The
quantity of analyte is determined by comparison to the
measurement of a reference standard curve determined in
the same assay. More details for SPR can be found in gen-
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
5674 〈1102〉 Immunological Test Methods / General Information
eral information chapter Immunological Test Methods—Surface Plasmon Resonance 〈1105〉.
Rate Nephelometry
Rate nephelometry is a quantitative method for measurement of an analyte in a sample in solution by measuring the
light scatter introduced by small aggregates formed by the
antigen–antibody complex. The quantity of analyte is determined by comparison to the measurement of a reference
standard curve determined in the same assay.
Radioimmunoassay
RIA, a sensitive ITM first developed in the 1950s, is a
quantitative method for measurement of an analyte in a
sample. RIA usually uses a competitive antibody–antigen
binding reaction, but it also can be used in sandwich immunoassay format, including immunoprecipitation. In competitive RIAs the analyte competes for binding with a radiolabeled (e.g., using 125I or 3H) reference antigen that is
identical to the analyte; therefore, the analyte and the antigen both compete for binding to a fixed and limiting dilution of a specific (often polyclonal) antibody. The radiolabeled antigen is present in excess. The same unlabeled
antigen in the test sample competes in binding to the same
site on the antibody, which is present in a fixed quantity.
Binding of the unlabeled antigen to the antibody leads to
the displacement of the labeled antigen, resulting in a decrease in the radioactivity of the antigen–antibody complex
fraction. To separate the antigen–antibody complex from
the excess unbound antigen, the complex generally is either
precipitated with a secondary antibody (or protein G) immobilized on a solid matrix (e.g., glass or resin beads) or
with an already immobilized primary antibody. The quantity
of analyte usually is determined by interpolation against a
standard curve of a reference material, where a fixed
amount of antibody and radiolabeled antigen is mixed with
an increasing amount of unlabeled antigen. Hence, even a
small quantity of unlabeled antigen will result in a relative
quantitative decrease in total bound radioactivity.
Single Radial Immunodiffusion
Single radial immunodiffusion (SRID or SRD) is a quantitative method for measurement of an analyte in a sample by
Second Supplement to USP 35–NF 30
measuring the diameter of the ring of precipitin formed by
the antigen–antibody complex. Antigen is applied to a well
in a gel infused with a constant level of antibody. Solutions
with higher concentrations of antigen diffuse farther before
being saturated with antibody and then precipitated. The
quantity of analyte is determined by comparison to a reference standard curve measured by the same assay.
Precipitation
The underlying principle for this method is that the interaction of a multivalent antibody and antigen leads to the
formation of a complex. In some cases a visible precipitate is
formed. Other immunoprecipitation techniques involve the
use of Protein A or Protein G beads to capture the
antigen–antibody complex and facilitate the separation of
the antigen–antibody complexes from the other antigens in
the solution. Precipitation is not commonly used for quantitative analytical purposes because of the time required (days
to complete), lack of sensitivity, and requirement for large
quantities of antigen and antibodies.
Agglutination
Agglutination and inhibition of agglutination, respectively,
provide qualitative and quantitative measures of certain antigens and antibodies. Inhibition of agglutination is a modification of the agglutination reaction that provides higher
sensitivity to detect small quantities of proteins, chemicals,
viruses, and other analytes. The principle of agglutination is
similar to that for precipitation except that the interaction
takes place between an antibody and a particulate antigen
and leads to a visible clump or agglutination. The most
common example of this application is for blood typing
(i.e., A, B, or O antigen).
CHOICE OF ITM
When choosing an ITM, analysts should consider sensitivity and specificity as well as the complexity of the sample.
Table 1 provides an assay developer with a comparative
view of the advantages and disadvantages of a variety of
ITM formats. The intended application of the ITM should
govern the choice of the most suitable format.
Table 1. ITMs Used in Biopharmaceutical Laboratories
Method
Advantages
High sensitivity
Often wide dynamic range
High throughput
Low cost
ELISA
•
•
•
•
Western
blot
• Gives information about antigen
size and/or charge
• Allows separation of various antigens (or degradation/aggregation
products) bearing same epitope
• Can tolerate complex mixtures
Flow
cytometry
• High throughput
• Highly automated
SPR
• Direct detection of binding
• Can measure affinity precisely,
including on and off rates
Disadvantages
• Multistage process highly dependent on proper execution of each
stage
• Wash steps add time and
often biohazardous waste
• Reagent labeling required
• Typically works only with linear
epitopes
• Labor intensive
• Low throughput, output
• Subject to interpretation
• Immobilization can alter binding
• Limited to proteins
• Use limited to cells, particles, and
samples bound to beads
• Sensitive to aggregates and sample
matrix
• Immobilization can alter binding
• Regeneration can alter binding
• Low throughput, output
Typical Industry Uses
• Potency assessment
• Specific protein concentration
analysis in complex samples
• Protein identification
• Purity assessment
• Immunogenicity assessment
• Protein purity assessment
• Protein stability assessment
• Protein identity test
• Potency assessment
• Cell identity in cell-therapy
products
• Immunogenicity assessment
• Potency assessment
• Specific protein concentration
analysis in complex samples
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
Second Supplement to USP 35–NF 30
General Information / 〈1102〉 Immunological Test Methods 5675
Table 1. ITMs Used in Biopharmaceutical Laboratories (Continued)
Method
Rate
nephelometry
RIA
Advantages
• Easily automated
• Rapid
• Binding occurs in native conformation
• Low-concentration samples can
be analyzed
• High sensitivity antibody used at
limiting dilution that conserves reagent
• Can be plate-based for higher
throughput (e.g., scintillation proximity assays)
• Precise
• Simple setup
SRD
Precipitation
• Low equipment cost
Agglutination
• Rapid
• Low equipment cost
Disadvantages
• Small detection range
• High background for turbid samples
• Requires radioactive labeling for
detection
• Shorter half-life of some radioisotopes requires periodic preparation of
the tracer
• Hazardous waste
Typical Industry Uses
• Assay for individual vaccine
components for check of stability
and purity
• Protein identification
(e.g., hormones)
• Specific protein concentration
analysis in complex samples
• Semiquantitative
• Low precision
• Low sensitivity
• Subject to interpretation
• Slow
• Poor sensitivity (µg range)
• Subject to interpretation
• Slow
• Low specificity because of interfering substances
• Vaccine release test
KEY CONSIDERATIONS IN ITM
DEVELOPMENT
The goal during method development is to produce an
accurate assay that is practically feasible and possesses an
acceptable degree of intra- and inter-assay precision. To
minimize the overall imprecision, the sources of variability
should be identified and minimized.
Reagent Selection
Immunoassays are subject to several sources of interference such as cross-reactivity, endogenous interfering substances, buffer matrices, sample components, exposed versus masked epitopes, conformation changes in the antigen
of interest, and other factors. Hence, during method development, analysts must identify possible sources of interference both to develop a robust method and to aid future
troubleshooting.
Cross-reactivity is a major obstacle during immunoassay
development. This arises when the specificity of an
antigen–antibody reaction is compromised by the cross-reactivity binding of structurally similar molecules with the reaction binder. Some common examples are protein
isoforms, degraded analyte entities, molecules of the same
class, precursor proteins, metabolites, etc. Cross-reactivity
can be minimized by rigorous reagent characterization and
selection.
Reagents used in ITM applications generally fall into one
of two categories: critical reagents and noncritical reagents.
Critical reagents are specific and unique to the particular
ITM or reagents that are intolerant of very small changes in
composition or stability. Examples of critical reagents generally include assay-specific antibodies and reference or
method calibration standards. Equivalence in the assay format must be established before replacement with a new lot.
Noncritical reagents are those that can vary to some degree
in composition without adversely affecting ITM performance. Reagents are often assumed to be noncritical
(e.g., buffers, water quality, blocking buffer, or substrate)
but later may be identified as critical components if assay
ruggedness fails and troubleshooting of ITM reagents begins. ITM-specific reagents, including vendor and catalog
number, should be defined in test procedure documents.
Antibody selection is critical for development of a successful immunoassay because it defines the assay’s specificity
• Vaccine identification
• Vaccine identification
and sensitivity. Furthermore, during antibody generation,
analysts should ensure that the immunization protocols support the end use of the antibodies. For some applications a
more specific antibody can be generated by the selection of
a small and specific immunogen and affinity purification of
the antibody, resulting in highly defined epitope coverage.
In other applications it may be critical to ensure broad coverage of the different available epitopes on the molecules of
interest, and a polyclonal antibody (pAb) pool may be the
best choice. Currently, monoclonal antibodies (mAb) are
preferred for some applications for the detection of single
analytes because of their high specificity, lot-to-lot consistency, and indefinite supply. Compared to polyclonal antibodies, mAb have a higher initial cost to produce, but for
these applications, the advantages generally outweigh the
initial cost. Other applications may require more comprehensive epitope selection to ensure that subtle changes in
the molecule(s) do not prevent recognition of the entire antigen, and thus a pool of monoclonal antibodies, or a pAb
pool, would be the preferred choice. The latter are widely
used for detection in a complex mixture of analytes (e.g.,
host-cell proteins). Similarly, immunoassays may use two
distinct epitopes on an antigen—one for capture and the
other for detection—which greatly reduces cross-reactivity.
Another approach to minimize cross-reactivity is to purify
the antigen before immunoanalysis. Variations in incubation
temperature and time can affect the reaction kinetics of antibody interactions with similar yet different antigens. Thus
this property should be optimized to increase the specificity
of antigen–antibody interactions.
Development of Immunoassays
Development is an important stage in the establishment
of a suitable ITM. During development of an ITM, analysts
explore various settings of assay parameters and interactions
between parameters to identify conditions under which the
assay will consistently produce reliable results using minimal
reagents, effort, and time. In Quality by Design terminology,
the “possible operating space” is the collection of settings of
assay parameters explored, and the “design space” refers to
the conditions under which the assay performs well. The
necessary performance properties of the ITM (precision, accuracy, specificity, etc.) required depend on the intended
use(s). During ITM development, analysts should consider
the following:
• Antigen–antibody ratio;
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
5676 〈1102〉 Immunological Test Methods / General Information
• In sandwich immunoassays, the ratio of capture antibody to detector antibody;
• Antigen–antibody reaction kinetics in the sample matrix
(antigen–antibody binding generally is not linear);
• Selection of the standard (full-length antigen for the
standard or just a small portion of the antigen containing the antibody-binding epitope, among other considerations); and
• Matrix effects.
The use of design of experiments (DOE) is strongly recommended, and different DOE methods may be appropriate in each stage of development. Early in development,
screening designs are particularly useful (generally two-level
geometric fractional factorial designs). After screening (with
a modest number of factors to study), full factorials or response surface designs are often appropriate. As development activities shift to qualification (ideally, if not typically,
as the focus shifts to robustness), robust response surface
designs often are a good choice. During qualification or validation, analysts may find it practical to simultaneously study
robustness to assay operating conditions (using a small geometric fractional factorial) and validation parameters such as
precision (via nested or crossed designs for random factors
associated with repeatability, intermediate precision, and
reproducibility).
Experiments that assess dilutional linearity and components of specificity, including matrix effects, usually involve
construction of spiked samples. Although spiking often is
performed in a dilution matrix, spiking a collection of actual
samples or mixing actual samples is an important component of demonstrating robustness of dilutional linearity and
components of specificity to the sample and matrix
components.
Reagent Considerations
A procedure for qualifying reagent sources and vendors
(including audits), ordering, receiving, and disposing of
commercial reagents and consumables should be outlined in
a standard operating procedure (SOP). The preparation of
internal reagents must be documented in a manner that
allows reconstruction. Commercial and internally prepared
reagents must be labeled with identity, concentration, lot
number, expiration, and storage conditions. The stability
and assignment of expiration dates for internally prepared
reagents often are based on available literature and scientific
experience, but analysts may need to confirm these empirically. An SOP for extending expiration dating of critical reagents is recommended. In addition, analysts should implement a mechanism for reagent tracking and linking lot
numbers to analytical run numbers. Unacceptable reagent
performance is detected by tracking QC samples. Shifts in
QC samples should prompt a review of analytical runs and
changes in reagent lot numbers or review of possible deterioration of critical reagents. To avoid such shifts, analysts can
cross-validate critical reagent lot changes.
The impact of collection and storage containers on analytical performance often is overlooked. When defining the stability and expiration of in-house reagents, analysts should
record information about the storage container vendor, catalog, and lot number. The importance of a suitable reference standard and its characterization cannot be overemphasized for ITMs for biological products. Because of their
inherent complexity, reference and calibration standards of
macromolecular biologics often are less well characterized
than are conventional small-molecule drug reference standards. If the calibration standard represents a mixture of different antigens (e.g., host-cell proteins), it should be shown
to be representative of the antigen profile in the samples
being tested. Consistency in ITM results depends on the
availability of a suitable representative reference standard
material.
Second Supplement to USP 35–NF 30
VALIDATION
Analytical validation involves the systematic execution of a
defined protocol and prespecified analysis that includes
prespecified acceptance criteria. A validation demonstrates
that an analytical method is suitable for one or more intended uses [see Validation of Compendial Procedures 〈1225〉,
Biological Assay Validation 〈1033〉, and ICH Q2(R1)]. Qualification may involve similar or identical experiments and procedures as validation, but qualification does not require
prespecified protocols, analyses, or acceptance criteria. In
certain situations (e.g., use of a commercial kit), assay development may not be required before qualification. General
information chapter 〈1225〉 discusses which assay performance characteristics must be examined during validation
for four primary categories of intended uses. For example,
analytical procedures that quantitate major bulk drug substances or active ingredients may not require validation of
the detection and quantitation limits but do require validation of accuracy, precision, specificity, linearity, and range.
System Suitability or Assay Acceptance Criteria
The purpose of system suitability or assay acceptance criteria is to ensure that the complete system—including the
instrumentation, software, reagents, and analyst—is qualified
to perform the intended action for the intended purpose. All
processes should be controlled by well-defined SOPs that
ensure consistency, reduce errors, and promote reproducibility of laboratory processes. Training files for all personnel
should be contemporaneous and should include some demonstration that analysts are qualified to perform the method
and the specific ITM.
Instrument and software qualification begins with a definition of the design qualifications, including a risk assessment
and gap analysis that identify potential threats to the collection, integrity, and permanent capture of ITM data. Qualification also includes installation qualifications (IQ) and operational qualifications (OQ). Purchased commercial
instrument validation packages may require modification to
meet the intended use at each facility. Instrumentation and
software should be continuously monitored for acceptable
functionality by performance qualification (PQ) and software
validation test script reviews. Routine instrument maintenance is performed according to the manufacturer’s recommendations, and additional maintenance may be required
based on specific needs in the working environment. A
complete history of routine and nonroutine instrument
maintenance should be archived for each instrument.
Software updates should be handled with change control
and typically require additional validation. Adherence to 21
CFR 11 should be maintained.
To ensure robustness, establish a defined process for implementing new ITMs in the laboratory. Control documents
should be in place, including method validation plans containing a priori method acceptance criteria and validation
reports for the establishment of a new ITM. Well-written analytical test method documents are needed to ensure reconstruction of analytical results and to minimize laboratory
errors.
Analytical test methods should include acceptance criteria
for critical aspects of the assay, including the performance
of the calibration curve, quality controls, agreement between sample replicates, procedures for repeat sample analysis, and identification and treatment of outliers, when applicable. Furthermore, an SOP should be implemented for
unexpected event investigation and resolution.
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
Second Supplement to USP 35–NF 30
General Information / 〈1102〉 Immunological Test Methods 5677
DATA REPORTING
Trending may detect shifts in assay performance that may
be related to events such as assay reagent lot changes, addition of new analysts, shifts in environmental conditions, and
others. SOPs, study protocols, analytical test methods, and
decision flow charts are recommended to strictly define the
handling, use, editing, rejection, acceptability, and interpretation of calibration data and test sample results for ITMs. It
is not uncommon to have several raw data reviews, including peer, QC, and quality assurance review. Analysts must
be able to distinguish such analytical issues from true
changes in the measured analyte caused by changes or errors in the manufacturing process that have affected the
product. Two of the most important outcomes of proper
trend monitoring are detecting potential problems before
they occur and identifying areas for corrective and/or preventive action. General information chapters Analytical
Data—Interpretation and Treatment 〈1010〉 and Biological Assay Validation 〈1033〉, as well as the statistical literature, contain guidance for various trending methods. Several ITM
performance characteristics could be considered for monitoring. The most common trending value is evaluation of
QC samples. Ideally, one or more QC sample is available for
long-term trending in sufficient quantity and with demonstrated stability so that quality aspects can be assayed in
every run and across multiple manufacturing lots. As the
long-term QC sample is depleted or expires, crossover comparison and establishment of a new long-term QC sample
should be completed. Systematic review of QC data across
assays assists in troubleshooting failed ITM runs, providing
confidence in the evaluation of spurious results, and controlling the introduction of replenished assay components that
may not perform exactly like previous reagents.
Other ITM performance characteristics that may be monitored include calibration curve response variables, curve fit
parameters, assay background, and comparison of in-study
QC data with validation data.
Units of Measurement
Quantitative ITMs generate test sample data with an estimated concentration based on a calibration curve fit to reference (or standard) samples using an appropriate mathematical model. When determining the amount of analyte in
a manufacturing process, analysts often express the unit of
measure in terms of mass of analyte per volume of solution
(concentration) or mass of analyte per mass of product
(e.g., parts per million). Depending on the nature of the
measured analyte, the degree of measurement standardization, the geographic region, and the history of the method,
analysts may express concentration in terms of weight per
volume, mole per volume, or weight of analyte per weight
of product. In some circumstances, concentration may be
converted to an activity unit of measure in which the
analyte mass is assumed to be 100% active. In certain circumstances, qualitative analysis using a predetermined cutoff value may be an acceptable alternative to quantitative
methods.
Immunoassay Data Analysis
ITMs employ calibration curves prepared with reference
standards of known (nominal) concentrations and are included in every bioanalytical method. This helps control variation associated with repeatability, intermediate precision,
and reproducibility and permits the estimation of results for
unknown test samples. Common simple statistical analyses
assume that the (possibly transformed) data are normally
distributed, have constant variance, are independent, and
that an appropriate model has been used. For many assays,
one or more of these assumptions may be inappropriate.
Analysts should assess these assumptions using a substantial
body of data (typically tens of assays). When these assumptions are not reasonable, the analysis becomes more
complex.
Calibration curves generally are characterized by a nonlinear relationship between the mean response and the
analyte concentration and typically are plotted in a log-linear manner with the (possibly transformed and/or
weighted) response variable (ordinate) plotted against the
nominal calibrator concentration (abscissa) in log scale. The
resulting curve that encompasses the assay’s validated range
is inherently nonlinear and often has a sigmoid shape with
horizontal asymptotes at very low and high concentrations
of analyte. Competitive ITMs have a negative slope, and
noncompetitive ITMs are characterized by a positive slope.
The analyte concentration in a test sample is estimated by
inverse regression against the calibration curve. The final result often is obtained after multiplication of the estimated
concentration in the assay by a dilution factor that is required to yield a response within the ITM’s quantification
range.
Under the guidance of a qualified biostatistician, analysts
can implement outlier tests in controlled documents that
permit the exclusion of spurious sample results. A well-defined procedure should be in place regarding how to identify, repeat, and report outliers. Outlier tests and interpretation of results are described in Analytical Data—Interpretation
and Treatment 〈1010〉. Test results that fall outside of their
predefined specifications or acceptance criteria should be
evaluated by an out-of-specification investigation to identify
a root cause.
Trending
A quality system includes monitoring of ITM performance
by collection and review of ITM performance characteristics.
Tracking
Regulatory agencies have strict requirements about maintaining the identity and integrity of both samples and data.
A quality process driven by SOPs must be implemented to
ensure the correct identity and integrity of test and reserve
samples. Ideally, a bar code system should be used to track
the collection, identity, location, chain of custody, number
of sample freeze/thaw cycles, storage temperature, and
length of time that a sample is stored. This information
should be captured and should be auditable from the time
of collection to disposal (or sample depletion). The ability to
track the sample history permits reconstruction of the events
leading to generation of a data result. This information is
used by regulatory agencies to ensure that the proper procedures were followed and by internal auditors to ensure
that pre-analytical sample handling did not compromise
study data. In addition, sample tracking allows a mechanism
for ensuring that the analyte measurement occurred within
the demonstrated window of stability for that analyte.
The final result generated from a bioanalytical laboratory
is a number that represents an analyte measurement in a
test sample. The steps necessary to generate that data and
preserve it in a report are numerous and are susceptible to
error. Therefore, quality systems must be in place to minimize data errors. Errors may be introduced by test sample
misplacement or identification, incorrect data reduction,
miscalculations, transcription errors, omissions, and other
factors. Ideally, validated software and laboratory information management systems are used when possible to generate, transfer, and archive data. Typically, redundancy checks
are built into automated processes by visual data review of
at least 10% of the data-transfer processes. In the absence
of validated electronic transfer, all data should be reviewed
by at least one reviewer. As with sample tracking, data generation, manipulation, and storage should be reconstructible. In addition, all data should be backed up using a
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
Accessed from 128.83.63.20 by nEwp0rt1 on Tue Jun 05 05:21:17 EDT 2012
5678 〈1102〉 Immunological Test Methods / General Information
format that is stable. Plans should be in place to update
archived data so that, as technology changes, archived data
can still be retrieved. Regulatory agencies require that raw
data be available for various lengths of time after the completion of a study or regulatory filing. Finally, data must be
secure from corruption, alteration, or access by unauthorized personnel.■2S (USP35)
Add the following:
〈1103〉 IMMUNOLOGICAL TEST
METHODS—ENZYME-LINKED
IMMUNOSORBENT ASSAY (ELISA)
■
INTRODUCTION
Immunological Test Methods (ITM) utilize binding between an antigen (Ag) and antibody (Ab). (See Appendix 1
for a complete list of acronyms used in this chapter.) Enzyme-linked immunosorbent assay (ELISA) is one of the
most widely used ITM for characterization, release, and stability testing of biotechnology products to help ensure the
quality of biological drug substances and drug products.
The term ELISA is used here in a broader sense and includes
enzyme immunoassays (EIA), as well as alternative detection
methods, e.g., chemiluminescence and fluorescence.
This chapter provides analysts with general information
about principles, procedures, experimental configurations,
assay development, and validation for solid-phase ITM like
ELISA and can be used for the other immunoassay variations mentioned above. The chapter also covers reference
standard(s) and control(s) used for immunoassays. The information can be adapted to the specific procedures of a monograph. This chapter does not cover immunoassays for the
measurement of immune responses to product in animals or
humans (e.g, serological or cellular assays), non-immunoassays (e.g, receptor-ligand interactions), or other related
approaches.
The chapter is part of a group of general information
chapters for immunological test methods [Immunological
Test Methods—General Considerations 〈1102〉, Immunological
Test Methods—Immunoblot Analysis 〈1104〉 (proposed), and
Immunological Test Methods—Surface Plasmon Resonance
〈1105〉], and also is related to the general information chapters for bioassays [Design and Development of Biological Assays 〈1032〉, Biological Assay Validation 〈1033〉, and Analysis
of Biological Assays 〈1034〉].
Second Supplement to USP 35–NF 30
ing its binding to an immunosorbent surface and its subsequent detection by the use of enzymatic hydrolysis of a reporter substrate, either directly (as with an analyte that has
enzymatic properties or is directly labeled with an enzyme)
or indirectly (by means of an enzyme-linked antibody that
binds to the immunosorbed analyte). Qualitative results provide a simple positive or negative result for a sample. Converting quantitative to qualitative results based on a cutoff
value that separates positive and negative results is common
practice. Because the performance properties of the assay
depend heavily on the cutoff value, the process used to determine the cutoff should be evidence-based and well documented. Quantitative assays determine the quantity of the
analyte based on the interpolation of a standard calibration
curve with known analyte concentration, run simultaneously
in the same assay. This standard should be an appropriate,
preferably homologous, reference or calibration material
that is representative of the analyte(s) of interest. The power
of immunoassays has been demonstrated by the variety of
procedures that have evolved, including alternative solid surfaces such as beads of different sorts, various plastics in
plates of different configurations, and alternative detection
methods, e.g., chemiluminescence and fluorescence. ELISA
assays are widely used in the biopharmaceutical industry for
various applications such as identity, purity, potency, detection or quantitation of antibody or antigen, and other
purposes.
Basic Principles
The essential steps of an ELISA can be broken down as
follows (see Figure 1):
1. Binding of the capture reagent (generally an antibody
or antigen), which functions as an immunosorbent for
capture of the analyte, to a solid surface;
2. Removal of excess, unbound capture reagent followed
by blocking of unoccupied binding sites with a blocking
protein such as albumin, gelatin, casein, or other suitable
material;
3a. Incubation of the analyte (in the test sample or reference standard) with the capture reagent to bind the
analyte onto the solid surface, followed by the washing
away of unbound material in the test sample and detection of the analyte. Direct detection occurs when the
analyte has enzymatic activity or has been linked to a
detector molecule (e.g., enzyme); or
3b. Incubation of the analyte (in the test sample or reference standard) with the capture reagent to bind the
analyte onto the solid surface, followed by the washing
away of unbound material in the test sample and subsequent detection of the analyte (Figure 1, step 3a). Indirect detection occurs when the analyte is detected by
the addition of a secondary enzyme-labeled reagent (Figure 1, step 3b); and
4. Quantification of the analyte by addition of a substrate suitable for the detector used (e.g., TMB, 3,3′,5,5′tetramethylbenzidine), followed by comparison of the
test sample to the reference standard.
Definition
ELISA can be defined as a qualitative or quantitative solidphase immunological method to measure an analyte follow-
Official from December 1, 2012
Copyright (c) 2012 The United States Pharmacopeial Convention. All rights reserved.
- Xem thêm -